Publication History
Submitted: December 05, 2021
Accepted: December 20, 2021
Published: January 01, 2022
Identification
D-0092
Citation
Peter John, Irina Yang & Aparna Goel (2022). A Systematic Literature Review of Importance of Emotional Competence in Healthcare Management. Dinkum Journal of Medical Innovations, 1(01):19-26.
Copyright
© 2022 DJMI. All rights reserved
19-26
A Systematic Literature Review of Importance of Emotional Competence in Healthcare ManagementReview Article
Peter John 1, Irina Yang2, Aparna Goel 3*
- Stanford Department of Medicine, Stanford, USA; peterjohn@stanford.edu
- China Medical University, Taiwan; Irinia_20981@cmu.edu.tw
- Stanford Department of Medicine, Stanford, USA; aparnagoel-90@stanford.edu
*Corresponding author: aparnagoel-90@stanford.edu
Abstract: It is thought that improving emotional intelligence is a prerequisite for improving leadership skills. Understanding the relationship between increased emotional intelligence and patient satisfaction, workplace engagement, and job happiness in healthcare personnel is crucial. This systematic review aims to explore the relationship between job and patient satisfaction, weariness, and work satisfaction, as well as the influence of emotional intelligence (EI) and communication skills on leadership. PRISMA guidelines were adhered to in order to perform a systematic search and review of the literature. Ten research were analyzed, with a focus on different facets of emotional intelligence. These research used a variety of scales and questionnaires to assess the connections between leadership, emotional intelligence, and other factors. A comprehensive examination of ten studies in all was conducted. Numerous facets of leadership and emotional intelligence have been studied, and the significance of this connection has been highlighted. Seven studies (or 70%) indicated a negative correlation between emotional intelligence and burnout. Six studies out of sixty percent of healthcare leaders revealed a positive correlation between emotional intelligence and job happiness. Higher levels of emotional intelligence in leaders translate into greater leadership, according to three studies (30%) that examine patient happiness. Increases in self-efficacy, empathy, job happiness, and patient satisfaction were all brought about by stronger emotional intelligence and better leadership. Higher emotional intelligence among healthcare professionals was also associated with lower burnout.
Keywords: emotional intelligence, leadership, healthcare
- INTRODUCTION
The ability to create feelings when they assist ideas, understand emotion and emotional knowledge, and regulate emotions to support both emotional and intellectual development is known as emotional intelligence, which is a subset of social intelligence [1]. There are three construct models of emotional intelligence that have been proposed: competency-based, ability-based, and non-cognitive models. It is believed that those with higher emotional intelligence (EI) are better able to recognize, understand, and control their emotions, which can improve their overall wellbeing and reduce emotional disturbance [2]. The demanding and ever-changing field of healthcare administration has made emotional intelligence a critical competency. The well-being of patients, the motivation of healthcare professionals, and the nuanced dynamics of human emotions fall under the purview of healthcare administrators, who oversee the intricate web of healthcare organizations. Emotional intelligence in healthcare administration is vital for the development of successful leadership, the advancement of patient-centered care, and the improvement of the complete healthcare experience. Residency programs should include interventions such as lectures and workshops to train residents and increase their emotional intelligence (EI). The patient-doctor interaction will be enhanced as a result of fewer mistakes and more patient satisfaction [3]. Worldwide research indicates that leaders should use their social skills to address issues as soon as they develop in order to resolve both potential and actual conflict with a patient. Developing relationships with coworkers may boost emotional intelligence (EI), which may have an effect on output on the job as well as employee happiness and retention [4]. Medical staff training and advances in diagnosis and treatment are important, but human contact is even more important, as over 40% of therapeutic outcomes are influenced by the patient-doctor relationship. It is easier for patients to describe symptoms to a doctor who understands their emotions, which improves diagnosis precision and leads to a clearer understanding of medical indications. It also gives a reliable tool for identifying the patient’s emotional states and directing them toward the most effective therapeutic approaches. Finally, it gives a chance to identify the patient’s wishes, opinions, or concerns regarding the illness and the course of therapy [5]. The significance of emotional intelligence in several facets of healthcare administration has consistently been highlighted in earlier research. According to these research, emotionally intelligent healthcare managers and professionals typically lead more successfully, form closer bonds with others, experience less stress and burnout, and make wiser choices. By examining the connection between these characteristics and attitudes toward organizational change, a study examined how emotional intelligence and the “big five” dimensions of personality can support organizational change at the individual level [6]. However, the results of certain earlier research may not be representative of the general population due to participant constraints. A small sample size raised the possibility of coincidental findings and decreased the results’ capacity to be generalized [7]. Response biases may have been established in research that evaluated leadership and emotional intelligence exclusively using self-report measures. Results of the Leadership Program may be erroneous or exaggerated as a result of participants giving socially acceptable answers or overestimating their own talents [8]. Our research aims to gain a deeper understanding of the effects of emotional intelligence on the dynamics of healthcare teams, specifically in terms of fostering a sense of unity within the team and a positive organizational culture that fosters increased job satisfaction, consensus-building, and open communication among healthcare personnel—all of which can ultimately lead to better patient care and clinical outcomes.
- MATERIAL AND METHODS
2.1 Study Design and Strategy
We conducted a systematic review in compliance with the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) and the stated guidelines and protocols for doing so. The available data and statistics on the topic are gathered, evaluated, and synthesized using a rigorous and methodical approach in the study design. We have searched a variety of internet databases, such as PubMed, Cochrane, Google Scholar, Science Direct, and PubMed Central, covering research conducted worldwide between January 2011 and March 2023. The particular search term that was used was as follows: The following: (Emotional Intelligence) OR (Patient Satisfaction) OR (Leadership).
2.2 Eligibility Criteria
Studies spanning a 12-year period were considered, and they included topics such as leadership, self-efficacy, empathy, work burnout, emotional intelligence, job satisfaction, and patient satisfaction, as well as how these factors relate to one another. Qualitative, longitudinal cohort, cross-sectional, and observational research were all considered. Excluded from the analysis were articles with only abstracts, systematic reviews, and articles that only addressed one variable. The following were eliminated: duplicate records, articles about leadership involving people other than healthcare professionals, and those without relevant results.
2.3 Study Selection
It was the responsibility of each author to determine whether or not a given article is appropriate for the study. They used predetermined eligibility criteria to independently evaluate the records, including the abstracts of these articles. The articles that passed this initial screening stage proceeded to the following round, where they were carefully examined in full text. This stage involved thorough inspection of every article.
2.4 Data Extraction and Synthesis
The year of the study, the nation in which it was conducted, the study design, the sample size, the study participants, and the main focus of the respective study—that is, the requirements of effective physician leadership, such as job satisfaction, self-efficacy, empathy, self-emotional appraisal, and patient satisfaction—as well as their relationships with various aspects of emotional intelligence—were among the data items that were extracted.
- RESULTS AND DISCUSSION
Our systemic review, which included ten qualifying research done globally, concentrated on several aspects of emotional intelligence that contribute to improved leadership among healthcare professionals. Elevated emotional intelligence was associated with significant increases in job satisfaction, empathy, and patient satisfaction. Employees who demonstrated a high level of self-emotional appraisal were also strong leaders with high emotional intelligence and experienced relatively less burnout. There was a range in sample size from 5 to 1195. Six out of ten research (60%) that addressed job happiness found that doctors with greater emotional intelligence scores had higher levels of career and life satisfaction. Seven out of ten research (70%) examined burnout, and there was a strong inverse relationship between work-related burnout and emotional intelligence. Three studies (30%) that addressed empathy suggested that having a strong emotional bond with patients and a critical component of empathy for subordinates are essential components of helpful leadership. Three studies (30%) that examined self-emotional evaluation, a crucial component of emotional intelligence, demonstrated its favorable correlation with leadership. Two studies (20%) that examined self-efficacy found that it positively correlated with emotional intelligence. Three studies (30%) that looked into patient satisfaction found that doctors and nurses with higher patient satisfaction scores also had better emotional intelligence.
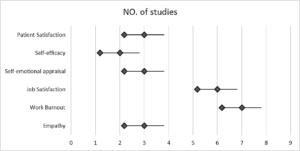
Figure 1: Demonstration of studies via forest plot
Table 1: Study Characteristics
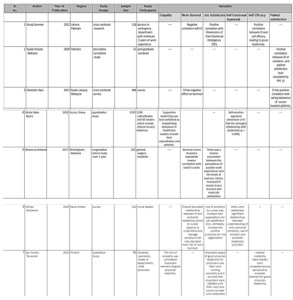
Effective and efficient healthcare service delivery, improved patient outcomes, and overall success for healthcare organizations all depend on leadership. Healthcare leadership encompasses a wide range of responsibilities, of which clinical leadership by physicians and nurses and administrative leadership by managers and administrators in the field are only two examples. According to certain research, there is no dominant leadership style among medical professionals, which emphasizes the need for leadership development and poses a significant challenge for healthcare workers in understanding how their behaviors as leaders impact performance [9]. Ten studies that looked at several aspects of leadership qualities—such as empathy, job satisfaction, burnout, self-emotional assessment, self-efficacy, and patient satisfaction—were included in this systematic review. These research emphasized the role that various emotional intelligence dimensions play in effective leadership. Six of the ten included studies addressed job satisfaction, and they all showed that doctors with greater emotional intelligence scores had better levels of career and life happiness. Maria Vakola et al.’s 2004 study revealed no conclusive evidence of a relationship between any emotional intelligence category and job satisfaction. 6. However, recent research has demonstrated that the two independent determinants of job satisfaction are pleasant work experiences and higher emotional intelligence [10, 11]. These results are consistent with a 2020 cross-sectional study by Ana Soto-Rubio et al. that found emotional intelligence to be a significant positive predictor of job satisfaction [12]. Seventy percent of the research found a significant negative correlation between emotional intelligence and occupational burnout. Five of the seven studies that found a negative correlation between work burnout and emotional intelligence also found that physicians who were burnt out had lower mean global EI than physicians who were not. The results are in line with what Kevin D. Cofer et al.’s study [13] discovered. The workload and administrative responsibilities of a leadership role may restrict how EI is expressed and manifested [14]. In one more of those seven research, we discovered that an overall favorable relationship between real leadership and emotional intelligence (EI) implies that nurses are capable of understanding and managing their emotions, which may lower their risk of burnout at work [15]. According to a study by Dana T. Lin et al., emotional intelligence scores were found to be a strong predictor of resident well-being 2. Emotional exhaustion (r = -0.69; p < 0.001) and depersonalization (r = -0.59; p < 0.001), and to correlate positively with psychological well-being (r = 0.74; p < 0.001) and inversely with depression (r = -0.69, p < 0.001). Three studies (30%) that looked at the subject of empathy found that having a deep emotional connection with patients and having empathy for subordinates are essential elements of supportive leadership [16, 17]. Keiko Abe et al.’s 2018 study on Japanese medical students found modest correlations between empathy and EI [18], but Meng Shi’s 2020 study revealed a favorable relationship between trait EI and empathy concern (p < 0.01) [19]. Three studies (30%) that looked into patient satisfaction found a positive correlation between EI and patient satisfaction attained by nurses acting with compassion for patients [20]. This result is in line with research by Hui-Ching Weng from 2008, which showed that patient trust was positively impacted by the physician’s EI (p <.05). The patient’s perception of the patient-physician connection improved and, consequently, the patient’s level of satisfaction increased (p <.01) with greater confidence toward the doctor.In [21]. Three studies (30%) that examined self-emotional assessment, a crucial component of emotional intelligence, found a positive correlation between it and leadership [16]. Understanding one’s own emotions, using emotion, and real leadership were all statistically significantly correlated [15, 27]. These results were in line with a review conducted in 2021 by Nerea Jiménez-Picón, which demonstrated how improving emotional intelligence (EI) in healthcare workers can raise their capacity to regulate their emotions, which in turn improves their resilience and the quality of care they provide [22]. According to similar findings in another study, transformational leadership requires leaders to be emotionally self-aware and able to control their emotions. Furthermore, personal EI competencies are a component of all transformational leadership components [23]. Two studies (20%) that addressed self-efficacy noted that medical credibility—that is, one’s competence—was seen as a necessary component of effective physician leadership [17, 24]. This result is consistent with the research of Leodoro J. Labrague, which found that motivation to lead (r = 0.343, p < 0.001) and leadership self-efficacy (r = 0.312, p < 0.001) are positively and moderately connected with authentic leadership [25]. These articles all emphasized the importance of emotional intelligence and the factors that influence it in terms of leadership. In order to hone their leadership abilities, medical students should also attend workshops and trainings. The majority of them are excited about an intermodal approach to leadership development that incorporates small group discussions, role-playing, and formal leadership courses that combine online learning with in-person instruction from professors (26].
- CONCLUSION
The contradiction between the urgent need for additional in-depth study on the subject and the support for emotional intelligence (EI) as a critical training skill in healthcare is brought to light by this review. Numerous research have demonstrated the impact of emotion usage and self-emotional evaluation factors on emotional intelligence and leadership. Higher emotional intelligence and effective leadership were linked to greater job satisfaction, patient satisfaction, empathy, and self-efficacy; conversely, lower burnout was observed among healthcare professionals with higher emotional intelligence.
REFERENCES
- Mayer JD, Roberts RD, Barsade SG. Human Abilities: Emotional Intelligence. Annu Rev Psychol 2008; 59: 507–536.
- Lin DT, Liebert CA, Tran J, et al. Emotional Intelligence as a Predictor of Resident Well-Being. J Am Coll Surg 2016; 223: 352–358.
- Waheed SS. Emotional Intelligence of Pakistani Doctors and its relationship with Patient Doctor Relationship. Health Prof Educ J 2020; 3: 41–47.
- Beydler KW. The Role of Emotional Intelligence in Perioperative Nursing and Leadership: Developing Skills for Improved Performance. AORN J 2017; 106: 317–323.
- Grubaugh ML, Flynn L. Relationships Among Nurse Manager Leadership Skills, Conflict Management, and Unit Teamwork. JONA J Nurs Adm 2018; 48: 383–388.
- Vakola M, Tsaousis I, Nikolaou I. The role of emotional intelligence and personality variables on attitudes toward organisational change. J Manag Psychol 2004; 19: 88–110.
- Bonazza NA, Cabell GH, Cheah JW, et al. Effect of a novel healthcare leadership program on leadership and emotional intelligence. Healthc Manage Forum 2021; 34: 272–277.
- Geun HG, Park E. Influence of Emotional Intelligence, Communication, and Organizational Commitment on Nursing Productivity among Korean Nurses. J Korean Acad Community Health Nurs 2019; 30: 226.
- Nizami R, Latif MZ, Hussain I, et al. Leadership Styles of Medical Professionals. Ann King Edw Med Univ 2018; 23: 508–513.
- Lindeman B, Petrusa E, McKinley S, et al. Association of Burnout With Emotional Intelligence and Personality in Surgical Residents: Can We Predict Who Is Most at Risk? J Surg Educ 2017; 74: e22–e30.
- Reed S, Kassis K, Nagel R, et al. Does emotional intelligence predict breaking bad news skills in pediatric interns? A pilot study. Med Educ Online 2015; 20: 24245.
- Soto-Rubio A, Giménez-Espert MDC, Prado-Gascó V. Effect of Emotional Intelligence and Psychosocial Risks on Burnout, Job Satisfaction, and Nurses’ Health during the COVID-19 Pandemic. Int J Environ Res Public Health 2020; 17: 7998.
- Cofer KD, Hollis RH, Goss L, et al. Burnout is Associated With Emotional Intelligence but not Traditional Job Performance Measurements in Surgical Residents. J Surg Educ 2018; 75: 1171–1179.
- Mansel B, Einion A. ‘It’s the relationship you develop with them’: emotional intelligence in nurse leadership. A qualitative study. Br J Nurs 2019; 28: 1400–1408.
- Alshammari F, Pasay-An E, Gonzales F, et al. Emotional intelligence and authentic leadership among Saudi nursing leaders in the Kingdom of Saudi Arabia. J Prof Nurs Off J Am Assoc Coll Nurs 2020; 36: 503–509.
- Apore GN, Asamoah ES. Emotional intelligence, gender and transformational leadership among nurses in emerging economies. Leadersh Health Serv 2019; 32: 600–619.
- Huikko-Tarvainen S. Elements of perceived good physician leadership and their relation to leadership theory. Leadersh Health Serv 2022; 35: 14–29.
- Abe K, Niwa M, Fujisaki K, et al. Associations between emotional intelligence, empathy and personality in Japanese medical students. BMC Med Educ 2018; 18: 47.
- Shi M, Du T. Associations of emotional intelligence and gratitude with empathy in medical students. BMC Med Educ 2020; 20: 116.
- Kaur D, Sambasivan M, Kumar N. Effect of spiritual intelligence, emotional intelligence, psychological ownership and burnout on caring behaviour of nurses: a cross-sectional study. J Clin Nurs 2013; 22: 3192–3202.
- Weng H-C. Does the physician’s emotional intelligence matter?: Impacts of the physician’s emotional intelligence on the trust, patient-physician relationship, and satisfaction. Health Care Manage Rev 2008; 33: 280–288.
- Jiménez-Picón N, Romero-Martín M, Ponce-Blandón JA, et al. The Relationship between Mindfulness and Emotional Intelligence as a Protective Factor for Healthcare Professionals: Systematic Review. Int J Environ Res Public Health 2021; 18: 5491.
- Küpers W, Weibler J. How emotional is transformational leadership really?: Some suggestions for a necessary extension. Leadersh Organ Dev J 2006; 27: 368–383.
- Sammer A. Emotional Intelligence and Self Efficacy as Predictors of Life Satisfaction among Doctors working in Emergency Department. J Dev Soc Sci; 3. Epub ahead of print 30 June 2022. DOI: 10.47205/jdss.2022(3-II)107.
- Labrague LJ, Al Sabei S, Al Rawajfah O, et al. Authentic leadership and nurses’ motivation to engage in leadership roles: The mediating effects of nurse work environment and leadership self‐efficacy. J Nurs Manag 2021; 29: 2444–2452.
- Imran N, Khalid B, Afzal Z, et al. Leadership in Undergraduate Medical Education: A Study of Pakistani Medical Students’ Perceptions, Attitudes, and Interest. Ann King Edw Med Univ 2023; 29: 105–110.
- Samiuddin KH, Ahmad I, Kazmi SZ. The role of emotional intelligence in hospital administration: a case study from Pakistan. Cross-Cultural Management Journal. 2017;19(1).
Publication History
Submitted: December 05, 2021
Accepted: December 20, 2021
Published: January 01, 2022
Identification
D-0092
Citation
Peter John, Irina Yang & Aparna Goel (2022). A Systematic Literature Review of Importance of Emotional Competence in Healthcare Management. Dinkum Journal of Medical Innovations, 1(01):19-26.
Copyright
© 2022 DJMI. All rights reserved


