Publication History
Submitted: February 05, 2023
Accepted: February 20, 2023
Published: March 01, 2023
Identification
D-0104
Citation
Sarah Rehman, Saira Rana & Mehru-Nisa (2023). Knowledge, Influence of Factors, and Management Strategies among Family Members with Behavioral Conditions. Dinkum Journal of Medical Innovations, 2(03):79-84.
Copyright
© 2023 DJMI. All rights reserved
79-84
Knowledge, Influence of Factors, and Management Strategies among Family Members with Behavioral ConditionsOriginal Article
Sarah Rehman 1*, Saira Rana 2, Mehru-Nisa 3
- Allama Iqbal Medical College, Lahore, Pakistan; sarahrehman90@aimu.edu.pk
- Allama Iqbal Medical College, Lahore, Pakistan; sairarana_khan@aimu.edu.pk
- Kinnaird College for Women University, Lahore; nisa-meharhamza@gmail.com
* Correspondence: sarahrehman90@aimu.edu.pk
Abstract: Mental health is becoming into a major issue of worry in the modern world due to the present paradigm shift. The World Health Organization estimates that 14% of all diseases are mental health disorders. Over 15 million individuals in Pakistan are estimated to be dealing with mental health issues. Mental health is becoming into a major issue of worry in the modern world due to the present paradigm shift. We have conducted cross-sectional study in 2022. According to a WHO estimate, around 14% of all diseases in the globe are mental health-related ailments. A recent study estimates that over 15 million people in Pakistan experience mental health issues and approximately 25% of Americans do as well. “Knowledge about mental disorders that aid in their detection, management, and prevention” is how the term “mental health literacy” (MHL) was defined in 1997.
Keywords: knowledge, influence, family members, behavioral conditions, management strategies
- INTRODUCTION
Mental health is becoming into a major issue of worry in the modern world due to the present paradigm shift. The World Health Organization estimates that 14% of all diseases are mental health disorders [1]. A recent study [2] estimated that over 15 million individuals in Pakistan are estimated to be dealing with mental health issues, while approximately 25% of Americans are assumed to be dealing with these conditions. “Knowledge about mental disorders that aid in their detection, management, and prevention” is how the term “mental health literacy” (MHL) was defined in 1997. Research indicates that individuals with greater knowledge about mental health are more likely to identify mental health issues and seek professional assistance for themselves and their family members [3–4]. There is a notable upward trend in mental health literacy across the globe. A small number of studies have examined mental health literacy, and there is a disparity between the number of cases recorded and the true prevalence of mental health problems in Pakistan [5]. Caregivers have a critical role in regards to patients’ mental health. In Asian culture, family members tend to the majority of those suffering from mental health disorders. The patient’s family helps the patient get necessary medical and psychiatric support, supplies, and keeps an eye on the patient’s mental health. These management initiatives are influenced by the mental health literacy of the caregiver. It is necessary to assess their understanding of mental health issues as well as all the factors that have an impact on their attitudes and propensities to seek assistance while managing mentally ill family members. The age, place of residence, level of education, socioeconomic class, and preferred method of initial consultation of the caregivers reveal information about their comprehension and perspective of sickness. The notion of societal stigma breeds mistrust about seeking medical attention. In a similar vein, people are discouraged from obtaining medical or psychiatric help due to misconceptions regarding the origins of mental illness, such as spirit possession and the evil eye [6]. Low mental health literacy is a result of a number of factors, including stigma, fear and mistrust of treatment services, financial limitations, cultural and religious views, and information gaps [7]. However, according to one study, 65% of patient attendants claimed to know the names of the illnesses that their ailing relatives had. Common illnesses include anxiety disorders, schizophrenia, and depression had low detection rates. Psychological and social variables are the most commonly cited causes of mental illness, as reported by patients and caregivers [8]. The bulk of research was done outside of Pakistan, and the studies that were done there had certain shortcomings in terms of fully examining all the factors that influenced people living in this area and the tactics they employed. The goal of this study is to close this information gap. It would determine how well-versed in mental health the caregivers are, especially with regard to what constitutes excellent mental health. By conducting a descriptive cross-sectional study to assess all the components of mental health literacy in the target group, it seeks to ascertain the various risk factors that prevent patients from seeking medical attention as well as their attitudes regarding the management of mental health problems.
- MATERIALS AND METHODS
This descriptive cross-sectional study was carried out at the Mayo Hospital’s psychiatry department in Lahore, the capital of Pakistan’s Punjab state. The study comprised the caregivers of patients with any kind of mental disorder who were admitted to Mayo Hospital Lahore. The investigation was carried out between June and September of 2022, and 160 patients were included in the analysis. The sample size was estimated with a 95% confidence level and 5% absolute precision. The selection of participants was done through convenience sampling. The included caregivers were all male or female members of the patient’s immediate family, ages ranging from 18 to 55. In cases where a patient had multiple caregivers, we requested the principal caregiver to volunteer to fill out the survey. The caregiver’s care for the patient must have lasted for a minimum of six months. The people included were just those who consented to give information. Those who were carers but had a diagnosis of any kind of mental disorder were not included. The relevant authorities granted authorization, and the study’s objectives were communicated to the participants. Once their approval was obtained, only those who voluntarily participated were included. Anonymity was maintained and the specifics of the personal data were kept confidential. The questionnaire was understandable to all. Through in-person interviews with the structured questionnaire, data was gathered. The first element of the questionnaire contained the sociodemographic data of the users. The “Public Perception of Mental Illness Questionnaire” was utilized in the second phase of the questionnaire to collect information on the caregivers’ understanding of mental health concerns [9]. There were thirty-three items on this questionnaire that tested the participants’ knowledge of mental illness (six items), the causes of mental problems (six items), their attitudes toward people with mental illness (twelve items), and how to manage people with mental health issues (nine items).
- RESULTS AND DISCUSSION
The socio-demographic makeup of the sample involved: 94 men (58.4%) and 67 women (41.6%) made up the respondents’ gender distribution, giving rise to a ratio of 1.4: 1 between males and females. The distribution of age was even. 37% had been widowed, divorced, or never married, while 63% were married. Just 27.3% of people resided in rural areas, with metropolitan areas housing the majority of people. 15.5% of those questioned had never attended school. The opinions of respondents regarding the genesis of mental disease are shown. The majority of respondents—about 82%—agreed that brain dysfunction causes mental illness. The claim that mental illness is brought on through hereditary inheritance was supported by 50% of respondents. And roughly 76% of respondents thought that substance usage contributed to mental disorders. As an alternative, around a third of respondents believed that mental illness was a punishment from God, while two-thirds believed that it was caused by something terrible that had happened to them. A personal weakness was cited by over a third of respondents as the cause of mental illness. In addition, more than three-quarters of respondents concurred that anybody can have a mental problem. More than fifty percent of those polled said that people who are mentally ill can work. Less than half of respondents, on the other hand, believed that those who suffer from mental health illnesses are mostly at fault for their disease. However, far fewer than half of the respondents said that the majority of the time, those with mental health problems is to be responsible for their condition. Few people assumed that a person with a mental disorder could truly develop friendships. More than 50% of respondents believed that individuals with mental problems may be identified by their looks. The survey’s responses were roughly evenly divided on whether people with mental illnesses are often harmful. Only one-sixth of the participants replied that people with mental problems must be avoided at all costs, while over half of the respondents thought that people with mental problems shouldn’t get married or have children. Only over half felt they may keep a connection with a person who suffered from a mental problem, but less than a fourth thought they might be married to someone who had one. A little less than half of those surveyed admitted that they may feel embarrassed if a member of the family had a mental disorder and that they might avoid speaking to someone who was mentally ill. Regarding therapy and care; almost the same number of participants disagreed with the point that mental problems cannot be healed and believed that someone may recover from it. According to two- thirds of the participants, families should not be kept in the dark about a person’s mental illness. Half of the respondents agreed that mental problems may be cured outside of the hospital, despite almost 66% of respondents agreeing that mentally ill persons must be in a department under monitoring. Only 36% of respondents believed that their PHC could effectively treat mental disorders, whereas 43% said there was awareness regarding mental illness there. However, two-thirds of respondents said they would be unable to share their mental health issues with anyone there. Software called SPSS-23 was used for the analysis. The association between the respondents’ education level and how they perceived the cause of the mental illness was examined (Table 1). When compared to respondents with lower levels of education, it was discovered that most respondents with matriculation and higher levels of education agreed that genes are involved in the course of mental illness. The majority of participants thought that drug misuse is a cause of mental illness. Among the illiterate, just 28% expressed disagreement. The majority of participants, both literate and illiterate, concurred that negative things happening to the individual create mental disease. While the majority of those with matriculation or higher levels of education disagreed, more than half of those with low levels of education said that mental illness is God’s punishment. The majority of those who disagreed were illiterate, while those with greater levels of education—80% of whom—agreed that mental problem is caused by a brain disorder. An inner weakness of the person is what leads to mental illness, according to two-thirds of respondents with low levels of education.
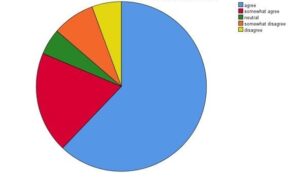
Figure 1: Mental Illness caused by brain disease
| Variables | education |
Total |
||||||
|
None |
Eleme-ntary |
middle |
matriculation |
Intermediate |
college/univer sity |
|||
| Genetic inheritance is the cause of mental illness | Agree | 5 | 3 | 4 | 11 | 6 | 14 | 43 |
| Somewhat agree | 6 | 3 | 5 | 5 | 4 | 14 | 37 | |
| Neutral | 2 | 3 | 1 | 7 | 1 | 1 | 15 | |
| Somewhat disagree | 3 | 2 | 5 | 9 | 4 | 8 | 31 | |
| Disagree | 9 | 6 | 6 | 6 | 2 | 6 | 35 | |
| Total | 25 | 17 | 21 | 38 | 17 | 43 | 161 | |
| Unfavorable life events may contribute to mental disease. | Agree | 16 | 13 | 15 | 21 | 11 | 34 | 110 |
| Somewhat agree | 1 | 1 | 1 | 7 | 5 | 8 | 23 | |
| Neutral | 3 | 1 | 2 | 2 | 0 | 0 | 8 | |
| Somewhat disagree | 2 | 1 | 1 | 2 | 1 | 1 | 8 | |
| Disagree | 3 | 1 | 2 | 6 | 0 | 0 | 12 | |
| Total | 25 | 17 | 21 | 38 | 17 | 43 | 161 | |
Although the study was carried out in Lahore, the socio-demographic features of this sample are more widely illustrative of all the communities because both the rural and urban populations are represented, rapidly and effectively. The findings of this study point to a lot of interaction with individuals who experience mental health issues, which may be caused by a high prevalence of disorders, insufficient services, a lack of communal acceptance of those with mental illnesses, or a sum of all three. This study urges more investigation. There are many different perspectives on mental illness in Pakistan, and many people stigmatize those who seek treatment, work, get married, or recover from a mental illness. Most people blame the sick person, avoid them, and are reluctant to talk about their psychological problems in public. Little studies have been conducted in poor nations, and the majority of assessments on knowledge of mental health have been carried out in countries in the west. Many people in Africa believe that supernatural causes are to – blame. According to a recent poll in Nigeria, confidence in biological and psychosocial causes of mental illness was connected with urban living, better educational status, and experience with the condition, but belief in supernatural causes was correlated with rural living. Western research has shown that biological factors (such as inherited factors and brain illnesses) and other factors (such as stress or trauma) are likely to be seen as responsible [10-14]. This study looked at how well-informed people who care for people with mental illnesses are about mental health. The few research studies that have been done in Pakistan to date have either concentrated on the association between first contact for therapy and superstitious beliefs in caretakers of people with schizophrenia or on traditional and religious methods of treatment that are still widely used, particularly in remote regions where mental health services are practically not present [15]. The attitudes and knowledge of the caretaker towards mental illness, however, are poorly understood. To better understand the caregiver’s mental health literacy, this study assessed the cause, understanding, mindset, and therapy of people with mental health disorders. The most common factors recognized as contributing to mental diseases, according to a study of community opinions on the subject conducted in Pakistan, were found to be a variety of socioeconomic variables. Nevertheless, neither a supernatural cause nor a biological explanation was universally accepted. According to the majority of caregivers in the current study, and line with earlier research, anyone can have mental health issues. Similar to earlier studies, the participants have negative views about mental illness, the blame is on the mentally ill patients, and they are unable to work or keep friendships [16]. The participants also had unpleasant opinions of mentally sick people. Both high-income and low-income countries have historically stigmatized persons with mental illnesses. According to the current descriptive study among recovered mentally ill, human rights abuses occur at the family and community levels, independent of gender [17], literacy [18], financial status [19], or place of residence. The current survey also exposes participants’ unfavorable opinions about mentally ill people’s social inclusion in the community. Participants admitted that they wouldn’t like others to get to know about their disease and that if they or a close relative were given a mental disorder diagnosis, they would be embarrassed. It proves that stigma and prejudice exist against people who have mental problems. About half of the individuals who participated in the current study reported feeling comfortable talking about mental health concerns that impacted them or members of their family, which is consistent with previous findings. Nonetheless, the bulk of studies discovered that patients frequently exhibited greater reluctance to reveal mental diseases to friends and family than physical disorders. Individuals in Pakistan have been seen to express their suffering in physical rather than psychological terms due to prejudiced attitudes.
- CONCLUSION
However, most people still stigmatize those with mental health issues when it comes to social contact, therapy, work, recovery, and marriage. The results demonstrate that participants with higher levels of education had a better understanding of the underlying causes of mental illness. * Therefore, there is a need for mental health literacy programs that target specific populations in need of mental health education, as well as public education and caretaker behavior modification on mental illness. Mental health professionals have an obligation to contribute responsibly to raising awareness of these particular communities.
REFERENCES
- Poreddi V, Blrudu R, Thimmaiah R, Math SB. Mental health literacy among caregivers of persons with mental illness: A descriptive survey. J Neurosci Rural Pract. 2015;6(3):335-60.
- Javed A, Khan MN, Nair A. Rasheed A. Mental healthcare in Pakistan. Taiwan J Psychiatry 2020;34(6):6-14
- Chen S, Wu Q, Qi C, Deng H, Wang X, He H, et al. Mental health literacy about schizophrenia and depression: a survey among Chinese caregivers of patients with a mental disorder. BMC Psychiatry. 2017;17(1):89.
- Mehrotra K, Nautiyal S, Raguram A. Mental health literacy in family caregivers: A compar- ative analysis. Asian J Psychiatry. 2018;31(2): 58–62.
- Pooja Agarwal & Komal Mishra. Examining the Long-Term Effects of Breastfeeding on Infants’ Neurocognitive and Gross Development. Dinkum Journal of Medical Innovations, 2(02):72-78.
- Tahir Jamil & Shamsa Mansha. Systematic Literature Review on Responsiveness and Readiness after Flooding: A Local Studyn. Dinkum Journal of Medical Innovations, 2(02):35-41.
- Muhammad Ayan & Ayesha Pervaiz Cheema. Patients’ Perceptions of Post-Mastectomy Mammary Reconstruction: Contributing Variables. Dinkum Journal of Medical Innovations, 2(02):42-49.
- Mutahara Ahsan & Mashal Ali. Systematic Literature Review on Individuals’ Satisfaction of Existence Affected by Bipolar Disorder. Dinkum Journal of Medical Innovations, 2(02):50-56.
- Anand Gopal & Nandita Shetty. Literature Review on Comparison of Efficacy and Safety of Mometasone Furoate 0.1% Gel Versus Mometasone Furoate 0.1% Cream and Adapalene Gel 0.1%. Dinkum Journal of Medical Innovations, 2(02):57-71.
- Angermeyer M, Matshinger H. Lay beliefs about mental disorders: a comparison between the western and the Eastern parts of Germany. Social Psychiatry and Psychiatric Epidemiology 1999,34(2):275-281.
- Gaebel W, Baunmann A, Witte A, Zaeske H. Public attitudes towards people with mental illness in six German cities. European Archives of Psychiatry Clinical Neuroscience 2002;252(18): 278-287.
- Stuart H, Arbodela-Florez J. Community attitudes towards people with schizophrenia. Canadian Journal of Psychiatry 2001,46(3):245-252.
Publication History
Submitted: February 05, 2023
Accepted: February 20, 2023
Published: March 01, 2023
Identification
D-0104
Citation
Sarah Rehman, Saira Rana & Mehru-Nisa (2023). Knowledge, Influence of Factors, and Management Strategies among Family Members with Behavioral Conditions. Dinkum Journal of Medical Innovations, 2(03):79-84.
Copyright
© 2023 DJMI. All rights reserved


